In grade 3 my best friend was diagnosed with leukemia. He frequently missed large stretches of class to receive chemotherapy. When he returned home I saw the result: hair loss, a puffy face, minor irritability. When I’d visit him I’d have to wash my hands extra good while his mom explained to me his different blood cell counts and what they meant for his treatment’s progress. But I was nine at the time and while I knew cancer was a major illness, I never fully grasped the magnitude of the event and never for a moment considered that my friend would lose his battle. Thankfully he survived his fight and to this day is fit as a fiddle, a testament to the power of modern medicine. And I think learning about my friend’s various drugs and treatments–both directly from him and from our school–helped convinced me that he’d pull through. A fundamental point we were taught by our teacher was that cancer isn’t contagious. To her credit she was mostly right: cancer cells from my friend’s bone marrow weren’t going to make the leap into me and give me leukemia. It was a good enough explanation for nine year old me and something I’ve always remembered. But if the title is anything to go by, what my teacher said isn’t the whole truth. Cancer, by way of viral machinery, could be called contagious.
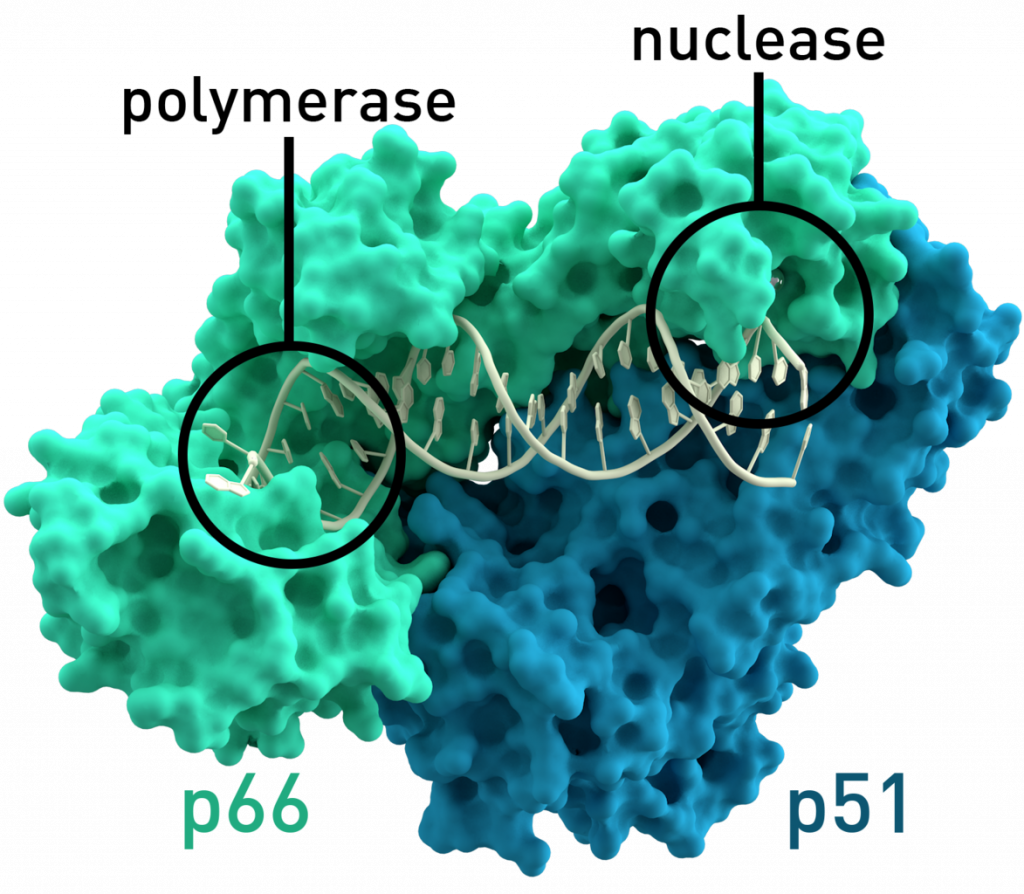
Space filling model of the viral reverse transcriptase enzyme. Credit: Thomas Splettstoesser (CC BY-SA 3.0)
Viruses encode their genetic information with either DNA or RNA. While DNA is resistant to mutation, for a virus it’s a bit of pain. To replicate their genes and produce mRNA, DNA viruses need to have their genome imported into the host cell’s nucleus in order for host polymerases to go to work. Freshly minted viral DNA and proteins then need to be coordinated in the cytoplasm before the viruses can leave to infect new hosts. The RNA viruses prefer a quicker, dirtier method of mass production. These virus are in perfect position to skip the host nucleus altogether and move directly to protein synthesis, using their genome as mRNA. Relying on RNA as genomic material is, however, risky; it’s chemically unstable and the host’s cytoplasm is jam packed with degratory enzymes and control mechanisms. A special group of RNA viruses called retroviruses come prepackaged with the enzyme reverse transcriptase, allowing their genes to be transcribed to DNA and then hidden within the host genome, awaiting the perfect conditions to strike.
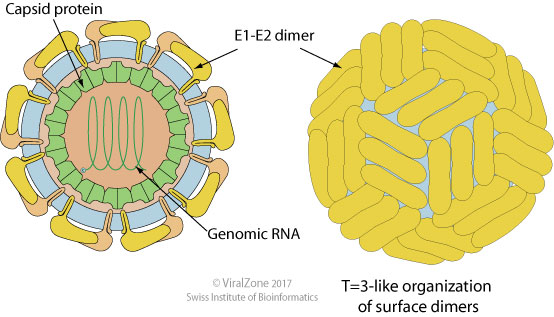
Diagram of Hepacivirus, responsible for Hepatitis C. Credit: ViralZone (CC BY-NC 4.0)
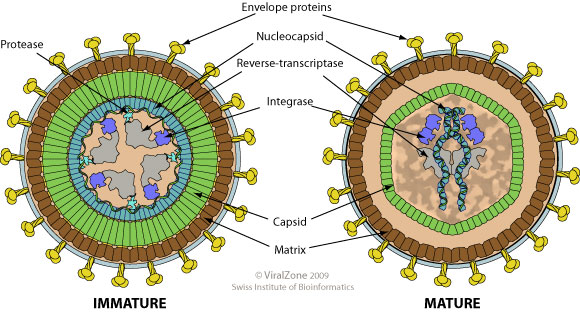
Much like with computer viruses, retroviruses hiding out in host genomes can wreak havoc upon cellular machinery. Two key examples are the Human T-cell Lymphotropic virus 1 (HTLV-1) and Hepatitis C virus (HCV). HTLV-1 was the first human retrovirus discovered after it was isolated from patients stricken with the highly aggressive cancer adult T-cell leukemia (ATL). It is thought that the main carcinogenic factor in HTLV-1 infections is a viral regulatory protein called Tax, which has the potential to induce immortality and rapid reproduction in infected T-cells. Tax likely, through direct protein interactions, upsets DNA repair pathways; coupled with the protein’s ability to speed up the cell reproduction cycle, this is the likely cause of cancerous T-cells. HTLV-1 is endemic to the African continent, Melanesia, and Japan. Thankfully, only about 2-4% of infections result in ATL. HCV, on the other hand, is a much blunter oncovirus which is transmitted through contaminated blood. A structural core viral protein has been implicated in a wide range of harmful actions, such as inducing oxidative stress leading to DNA damage, inhibiting cyclin modulators resulting in runaway cell replication, driving cell death through apoptosis, and knocking out the tumor suppression gene p53. Chronic infections of HCV are therefore highly damaging to the liver, causing cirrhosis in as many as 20% of cases. It is from both the physical damage of cirrhosis and the cellular damage from viral core protein that results in liver cancer.
Structures of HTLV-1. Credit: ViralZone (CC BY-NC 4.0)
Killing some 550,000 people worldwide annually, the sexually transmitted Human Papilloma virus (HPV) accounts for five percent of cancers worldwide and is perhaps the greatest example of a ‘contagious’ cancer. Two specific strains of HPV are responsible for nearly all cancers caused by the virus: HPV 16 and 18. Unlike the two retroviruses described above, HPV is a double stranded DNA virus. The DNA is packed within the viral capsid as a single loop wound around histone proteins in a gross imitation of eukaryotic chromatin. Another quirk of this virus is its ability to occasionally integrate itself into the host genome even though it isn’t required for reproduction. Much like the retroviruses, integration messes with signalling pathways and, in the case of HPV, confers immortality to infected cells. Tumor suppressant protein p53 is again a primary target with two possible pathways by which HPV eliminates it. Firstly, integration could disrupt the action or regulation of c-myc, a key gene regulator, which in turn imbalances p53 levels. Secondly, two viral proteins carried by HPV called E6 and E7 have wide ranging effects. This pair of proteins have been found to bind and inhibit p53 and additional tumor suppressants, break interferon regulators, disable certain transcription factors, and mess with certain histone remodeling proteins. While it is estimated that between 10-20% of infections result in cancer, vaccines are available to protect against several strains, most notably 16 and 18. Capsids featuring surface proteins, but lacking any viral DNA, are injected into the recipient, causing the immune system to mount a response with HPV specific antibodies; an effectiveness rate approaching 100% is reported.
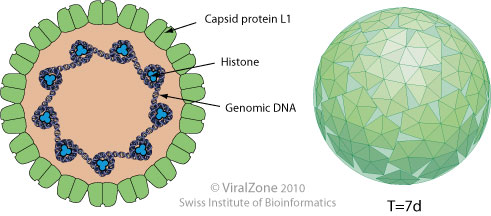
Generic structure of the viral family Papillomaviridae, which includes HPV. Credit: ViralZone (CC BY-NC 4.0)
At the end of the day, my grade 3 teacher was technically correct: cancers aren’t directly transmissible. That being said, the three oncoviruses explored above very much are transmissible. Through their complex machinery they upset the balance in their host cells and can confer hideous immortality. Cancer is complex–we’ve only just peeked in on the method behind the madness.
Recent Comments